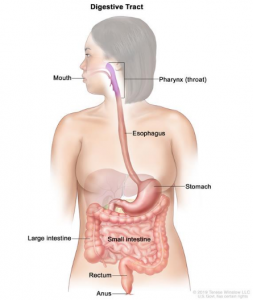
When it comes to perinatal bowel dysfunction, mum’s the word…or, at least it was. Women are either shy to mention their bowel habits or they’ve been told “Oh, that’s just normal. It’s a part of the process!” We’ve come too far in the field of women’s health to accept that answer. We can be proactive, even if certain issues are ‘part of the process.’ As a pelvic health physical therapist, I am here to tell you that you don’t need to suffer in silence. Bowel functioning is an important part of quality of life and overall health, and it can be the driver for low back pain, pelvic girdle pain, pelvic floor dysfunction, fatigue, and many other things. While it is beyond the scope of this blog to do a deep dive into the pathophysiology of how constipation begins in prenatal women and continues into postpartum, I want to share the simple things that CAN be done whether you are in the prenatal phase or your postpartum months.
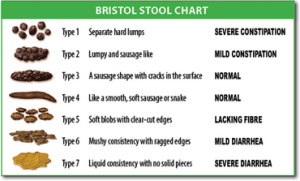
- Discern onset of constipation behaviors. Early on in postpartum period, some women are afraid to poop! They’ve had trauma, pain, etc and anything that exits the body can be scary, not to mention it can feel like your insides are going to fall out. This lays the groundwork for constipation patterns to begin. Fear + pain = backing up of pipes. If stool sits in the descending colon for too long, more water gets pulled out, making the stool hard and doubling up on constipation and other bowel troubles. You can assess the health of your stool using the Bristol Stool Chart. Deep breathing, drinking ample water and eating veggies (fiber, fiber, fiber!) can help improve stool quality and reduce constipation. Squatty potties can help (see #3). But we need to recognize when constipation patterns begin so we can be proactive.
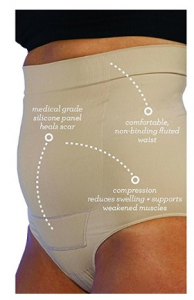
- Promote early tissue healing. Rest, ice, compression. Within 2 weeks of any surgery, medical providers would never send someone home and not give them proper tissue healing education. We should treat women who have had c-sections or vaginal deliveries just like any other patient! Icing can help relieve tissues of acute discomfort (i.e. a frozen water bottle on the perineum). Also, using support and compression. Donning a great pair of maternity underwear with a pad can help support the tissues, just like a brace for the knee or ankle does (FYI- there are incredible compressive support garments on the market that help lift and support the perineum postpartum). And rest. Easier said than done for new moms, but in general, give yourself permission to ‘rest’ in order to come down from the high of childbirth. This helps the GI system reboot and enter rest/digest parasympathetic mode.
- Potty position. The Squatty Potty is a fabulous invention. It promotes gentle knee/hip flexion while on the ‘potty’, which helps improve the pelvic floor muscles’ abilities to relax in order to have a bowel movement. Fun fact: the Squattypottymus is great for kids struggling with constipation.

- Chew, chew, chew your food. You’re a busy postpartum mom with one, two, three kids (or more!) and the last thing you have time to do is eat…much less actually chew your food. But it’s such a simple thing to do if you’re struggling with constipation. Eat even if you have to eat when you’re breastfeeding. Simply eating and chewing correctly gets digestive enzymes going down track and stimulates the GI system to get busy.
- Magnesium. It’s no secret that magnesium helps us poop. Consume foods that are rich in magnesium to promote digestion. Check with your OB, midwife, or whomever is on your birth team to see if you need a jump start (Miralax, magnesium citrate, etc).

- Consult with a pelvic health physio. Pelvic health physical therapists can assess your pelvic floor muscles and help you find ways to relax your pelvic floor muscles. They can assist with better ways of moving, teach you how to bear down to have a bowel movement, and help you work with scar tissue and abdominal wall massages. They can also support you in resuming the proper level and type of exercise that pertains to you as an individual and can meet you where you are at in your phase of healing.






